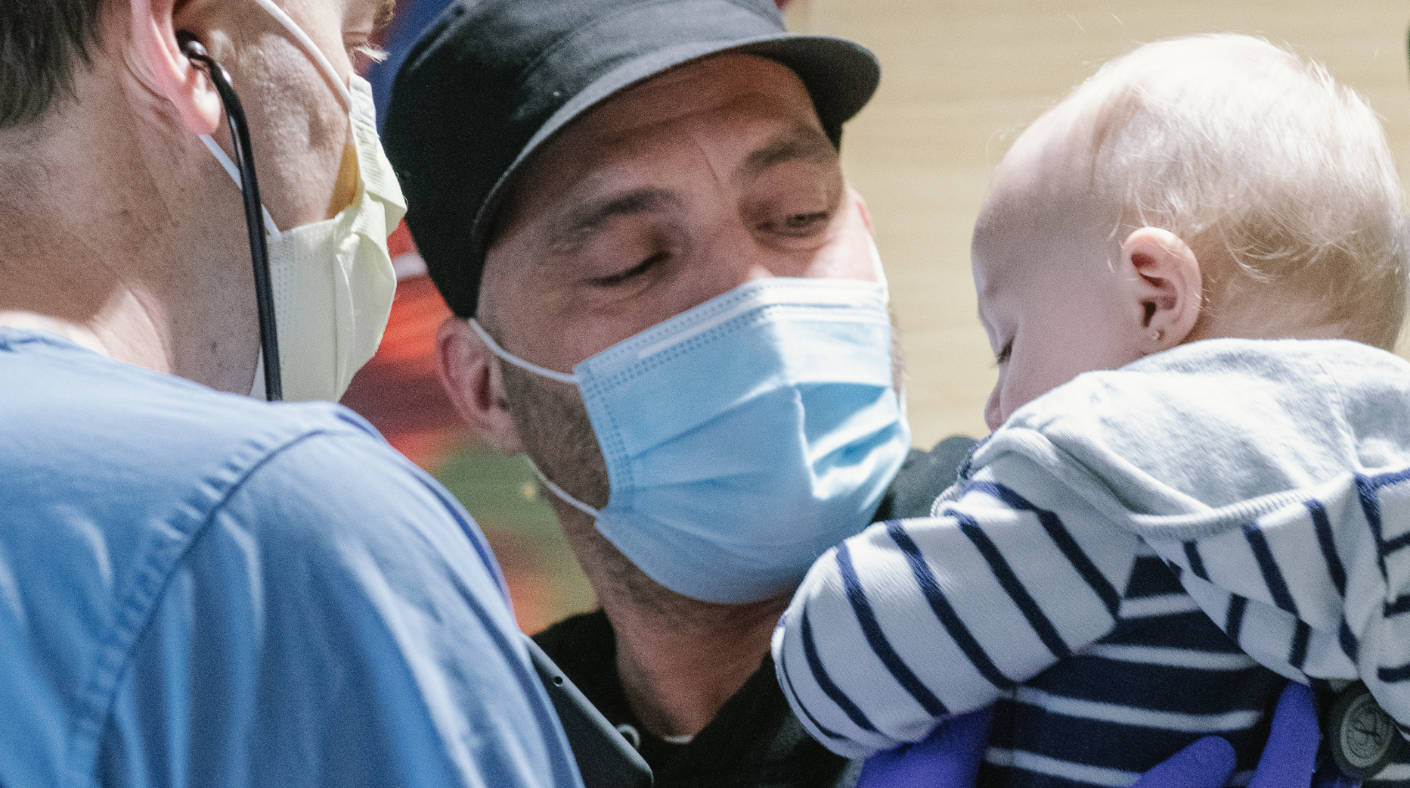
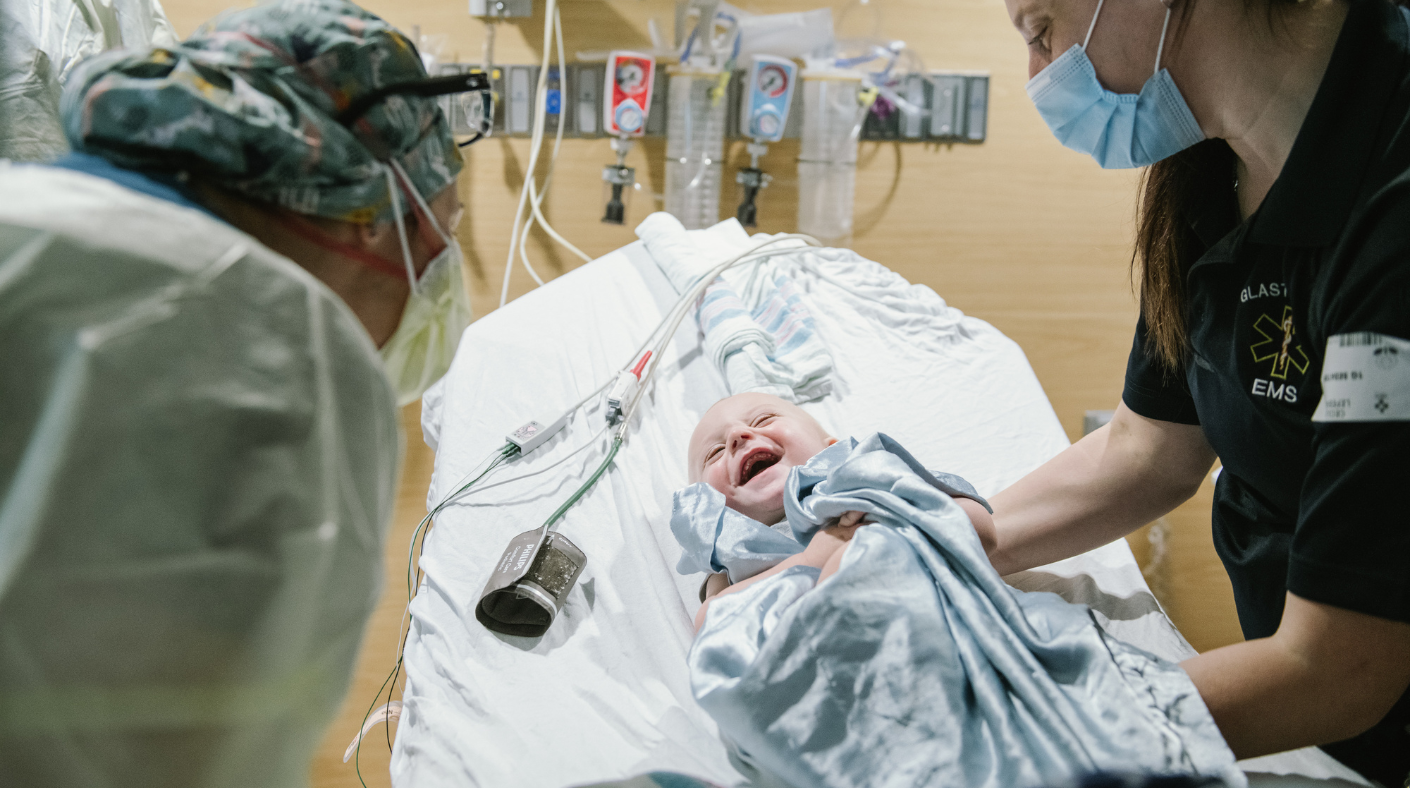
Sedation Services may not get as much public attention as Cancer or Cardiology, but it is a godsend for many patients and families. When a child needs to undergo a procedure that might be uncomfortable or intolerable but does not require full general anesthesia, sedation offers a helpful alternative. Sedation relaxes the child and makes him or her insensitive to what is happening without being completely unconscious. And it is usually combined with pain medication. Sedation is essential for painful procedures and can be helpful for even very minor procedures, like an exam, if, for example, the child cannot stand to be touched or is autistic. It’s also used for patients who are getting an MRI or CT scan and may be frightened. The overriding theme of the Sedation Center is compassion—to ease children’s anxiety and avoid pain. And it’s working: Connecticut Children’s Sedation Services has been named a Center of Excellence by the Society for Pediatric Sedation, the only such center in the state.
To get a better sense of what goes on in Sedation Services, we spent a day there. Here, we present some glimpses of the activities that went on during that day.
Latest Articles

Can More Be Done to Help Kids Heal After Surgery?

Changing the Future of IBD Care with Gut-on-a-Chip