It was a perfectly normal day four and a half years ago when Jean was picking up her four-month-old daughter, Mona, at daycare. But Jean sensed there was a problem.
“She wasn’t right,” she says. “She was having these little episodes. We couldn’t put our finger on them, but we knew she was not right. We ended up at one of the local children’s hospitals having these continuing episodes, and no one could identify what was happening. Finally, a new provider came on and said, ‘Wait a minute, she’s having a seizure.’ In that minute, our lives totally changed.”

Knowing that Mona was having seizures was only the first step. The next thing was to figure out why and what to do about it, and no one seemed to have those answers. “Our good days were great,” Jean says, “but when we had bad days, man, we had bad days. Nothing seemed to work in controlling the seizures and she was maxing out on all the seizure medications. She was bounced around from specialist to specialist trying to make sense of it all. We got second, third, and fourth opinions from all these children’s hospitals.”
It wasn’t until Mona was eight and a half months old, when her genetic testing came back from the lab, that answers finally came: Mona, they discovered, has two genetic deletions in her DNA. The most significant one is a gene called SCN1A. Kids who have a mutation in this gene develop what’s known as Dravet syndrome, a rare and severe form of epilepsy that produces frequent, major and difficult-to-control seizures. Because Mona is completely missing that gene rather than having a mutation in it, her symptoms are not perfectly aligned with a Dravet diagnosis. Still, Dravet syndrome is the closest thing to a diagnosis anyone has been able to come up with, and it gives her medical team a place to start.
In addition to seizures, Dravet can result in developmental delays and other problems. In Mona’s case, those developmental delays are compounded by her other gene deletion, SCN1B. Mona has very low muscle tone and is not ambulatory. She’s in a wheelchair. She doesn’t eat by mouth and has a feeding tube for her nutrition. She’s also nonverbal. “She doesn’t use words,” Jean says, “but she sure knows how to communicate with her eyes.” In addition, her low muscle tone means she has frequent respiratory issues. “She recently had a common cold,” Jean says, “and she was in the hospital for two weeks.”
She doesn’t use words, but she sure knows how to communicate with her eyes.
Jean Z., Mona's Mother

Because the seizures can be so severe with Dravet syndrome, Mona is in a high-risk group for SUDEP, or sudden unexpected death in epilepsy.
“The seizures that are most concerning are tonic seizures,” says her neurologist, Jennifer Madan Cohen, MD, who is the medical director of Connecticut Children’s Epilepsy Center and the Neurodiagnostics Lab Center and who works with the Ketogenic Diet Program. “In these seizures, her whole body becomes as stiff as a board as her muscles contract. That includes the chest wall muscles that move her lungs. And these seizures can last for three minutes.”
In addition to the two gene deletions, Mona has something called secondary adrenal insufficiency (your adrenal glands produce hormones that regulate your metabolism, immune system, blood pressure and other essential functions). “Day to day,” Jean says, “her adrenal function is near perfect, but with an illness or a stressor to her body, she becomes adrenal insufficient and needs a pretty high dose of steroids to keep her body doing what it needs to do.”
As you can imagine with these symptoms and conditions, Mona requires constant attention. “She is never alone,” Jean says. “She requires at least one adult eye on her all the time, and it has to be someone who knows her really well.”
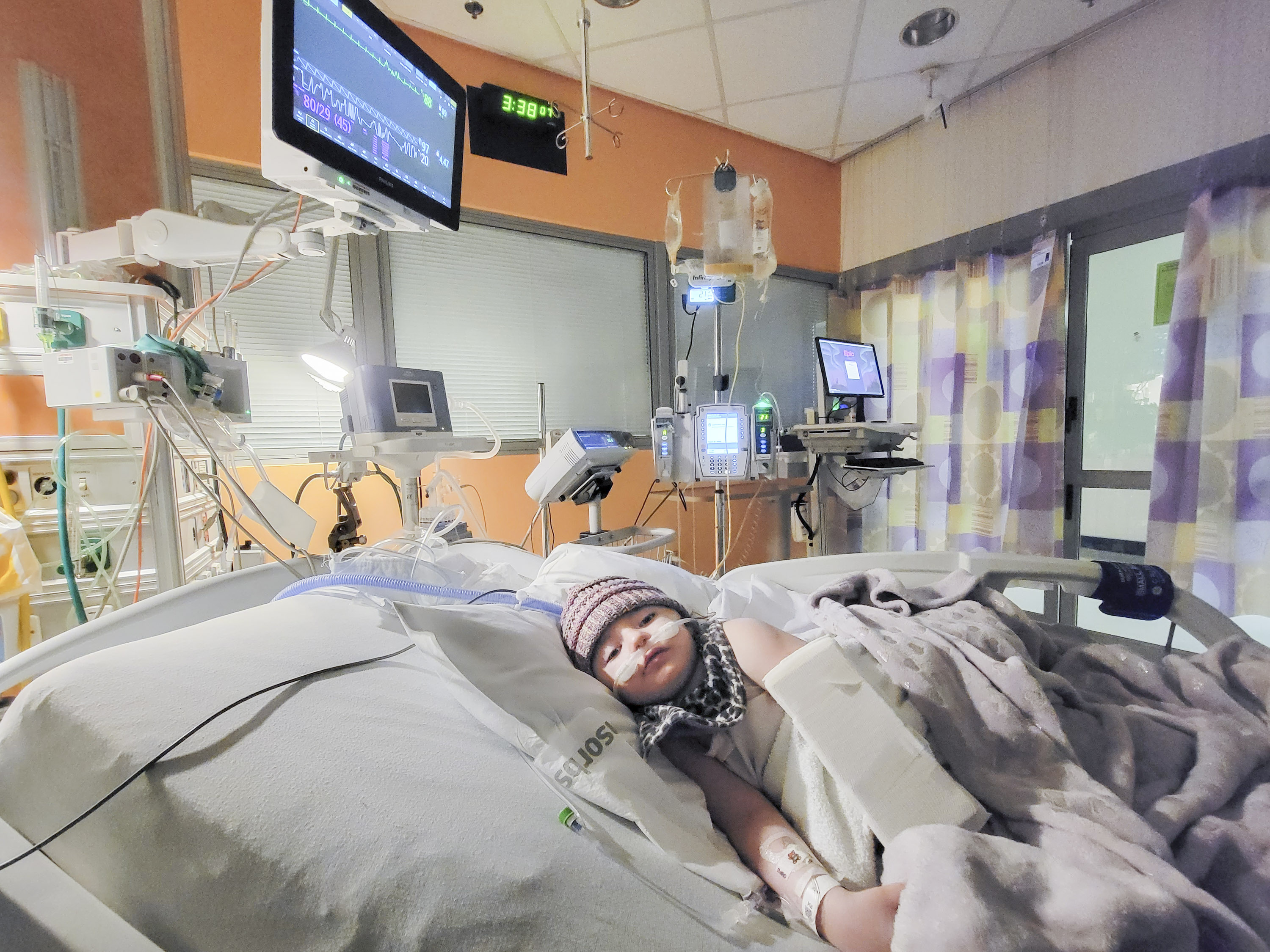
So Jean and her husband have to work on opposing schedules. “Dad is home with her during the day,” Jean says, “and then we are two ships passing in the sea. As I get home from work, he’s getting himself ready. He leaves usually between 4:00 and 4:30, and then he comes home in the middle of the night.”
To treat the two gene deletions and control the seizures, Dr. Madan Cohen is currently giving Mona four different drugs. Figuring out which drugs in which doses will work for any given patient with Dravet syndrome is challenging. She would like to decrease or even eliminate one of the drugs because it is causing problems with Mona’s red blood cell count. But when she tried to eliminate it earlier, the seizures worsened. So now she is thinking of trying to decrease the dosage slowly. It’s all a matter of balancing risks and benefits. There is no quick fix.
For Mona’s parents, the glue that holds this all together is love. “We have seen her through several days where we were doing one day at a time down to one hour at a time to one minute at a time. We were just looking at that clock, hoping to make it to 6:02 and then 6:03. Then comes 7:15 and she opens her eyes and gives us the most breathtaking smile that you could ever imagine. We were just sure that it couldn’t ever feel any worse than this, or it couldn’t feel any harder, and she just takes it away. I’m not sure where she takes it, but she takes it right from us. And she puts it somewhere that is so special.”
All-Stars Patients
Latest Articles

Can More Be Done to Help Kids Heal After Surgery?

Changing the Future of IBD Care with Gut-on-a-Chip
