Marilyn Sanders is the medical director of the Neonatal Critical Care Transport Program. This program uses a highly specialized ambulance team to bring sick newborns to Connecticut Children’s’ Level 4 or Level 3 Neonatal Intensive Care Units (NICUs) from other hospitals in the state that may not have the facilities or specialized clinicians a given child may need. We sat down with Dr. Sanders to learn more about the program and her involvement in it.
Latest Articles

Award-Winning Connecticut Children's Foundation Gala Reveals 2026 Theme
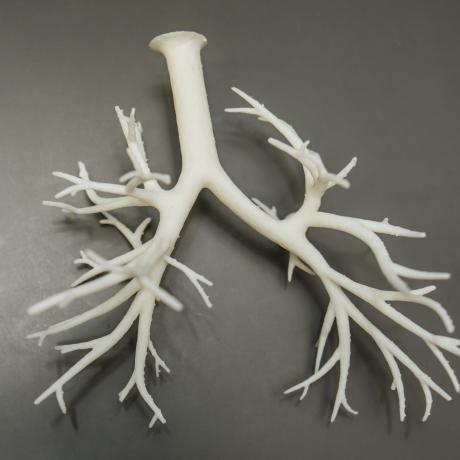
Printing Hope in the Lab